The Untold Toll of Medicaid Unwinding
By Naomi Fener, Kiersten Zinyengere,
04.08.2024
With the end of COVID-19 public health emergency-induced flexibilities, nearly 20 million people have lost Medicaid health insurance coverage. Some of these losses were due to those who were found to be no longer be eligible for the program, but many lost their coverage due to procedural errors, capacity issues, overburdened Medicaid offices, and Churn.1
Health insurance access has a significant impact on a person’s overall health and Medicaid unwinding will without a doubt have long-term health implications for many of our most vulnerable Americans. Without coverage, people will limit or delay medical care and neglect filling important and often lifesaving prescriptions.
Medicaid is known as the largest public insurance program for children, seniors and individuals with disabilities, and it does so much more than just provide health care access. It connects people and families to broader services and supports that help keep them and their communities healthier. Unfortunately, the direct impact on access to health care services is just the tip of the iceberg: the long-term effects of Medicaid unwinding will have broad impacts on individual and population opportunities for health and well-being.
The Unequal Coverage Loss Burden
It is especially important to note that these coverage losses and the resulting long-term impact are not experienced universally across populations. Medicaid covers a disproportionate share of people of color, thereby putting communities of color at particular risk of losing access to key services and support.
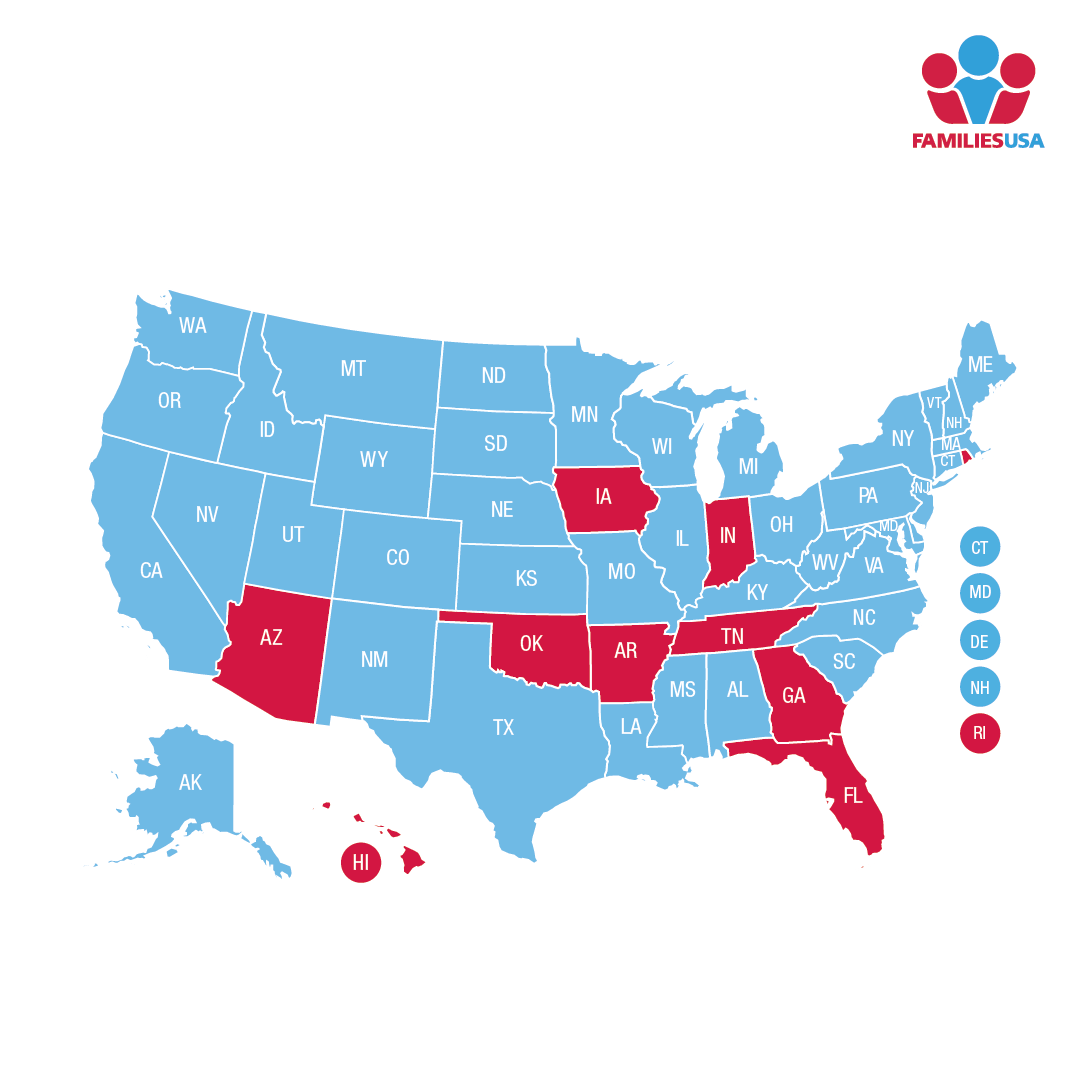
However, as of September 2023, only nine states reported Medicaid disenrollment data that included race and ethnicity.2 The reported data has limitations due to differences in collection, and how race and ethnicity are defined. While this limited data does not show significant racial disparities in disenrollments, this is an extremely narrow view into the current situation, and unwinding could further exacerbate longstanding racial and ethnic disparities. The Assistant Secretary for Planning and Evaluation predicted that Latino and Black individuals, and children and young adults in particular, will be disproportionately impacted. Their analysis predicts that 35.3% of Latinos, 15.1% of Black, 57.1% of children and 12.1% of young adults disenrolled despite remaining eligible.3
While these are only predictions, we do not need to wait for more comprehensive breakdowns of data to see that there are disparities. Even the limited data we have from states reporting racial and ethnic data shows Hispanic children had the highest rate of disenrollments, from 5.2% to 12.5%.4 Policymakers should act now to ensure that historically marginalized communities are receiving extra outreach and attention during disenrollments.
When Health is More Than Health Care
When we think of Medicaid, we often think of covering the cost of doctor’s visits and medications, but for many, Medicaid provides so much more. Medicaid offers financial protections like limiting out-of-pocket costs, and often covers additional services beyond traditional health care, such as housing and employment supports, and nutrition or food security services.5
The World Health Organization (WHO) estimates that 30–55% of health is driven by non-medical factors such as the social drivers of health (SDOH).6 To address SDOH (or the conditions in which people live, grow, learn, and play), and the related health impacts, many state Medicaid agencies are implementing programs to address those factors including housing, nutrition, heat, electricity, and transportation supports, to name a few.
State Medicaid agencies are more frequently utilizing 1115 waivers to address SDOH. As of March 1, 2024, 18 States utilize Medicaid waivers for housing supports, eight for nutrition supports, five for employment supports and four for Medical respite; many other states have similar waivers pending.7 For people who lose their coverage during the unwinding, the loss of Medicaid will also result in the loss of access to these vital services.
Financial Impact
Medicaid does not just improve the physical and mental health of its beneficiaries, but improves financial health as well.8 Medicaid expansion was credited with reducing the bankruptcy filing rate from 2008 to 2017 and other research found that Medicaid enrollment is associated with improved financial health through reducing unpaid bills, credit card spending and evictions, judgements and bankruptcy.9 10 Medicaid expansion reduces income inequality especially amongst racial/ethnic groups and individuals with lower educational attainment, giving millions of hardworking beneficiaries the chance to experience financial stability.11
The financial impact is well illustrated in the 2008 Oregon Experiment, where researchers tracked clinical and non-clinical outcomes as Medicaid was expanded in the state.12 While many of the new enrollees were relatively healthy at baseline, resulting in less impact on clinical outcomes, there were significant impacts on health-related quality of life. Participants with expanded access to Medicaid increased their use of health care services, the detection rate of diabetes was raised, rates of depression were lowered, and financial strain was reduced overall.
Housing Impact
Medicaid provides a level of financial security that keeps people from having to make the difficult choice between having a roof over their heads and paying for their families’ health. There are not many other programs that demonstrate that level of success. History shows that when people lose their Medicaid coverage, the impacts on safe and secure housing are severe. In 2005, Tennessee underwent a large Medicaid unwinding. In addition to decreased utilization of the health care system, the TennCare disenrollments were associated with a 27.6% increase in the average annual eviction filings and 24.5% increase in completed evictions.13
While there was not analysis of racial disparities in evictions at the time, we know that significantly more White families own homes compared to Black and Hispanic families, as of 2022.14 The loss of financial stability and housing supports through Medicaid will have compounding impacts on Black and other people of color.
Maternal Health Impact
Racial and ethnic disparities in maternal mortality (defined as a person’s death during pregnancy or in the year after giving birth) are widely documented and significantly worsened during the COVID-19 pandemic.
Pre-pandemic, pregnancy-related Medicaid eligibility (generally 200% of the Federal Poverty Level (FPL) vs 138% for other people, though this varies by state) meant that a person with income greater than 138% FPL would lose pregnancy-related Medicaid eligibility and coverage just 60-days postpartum. This would leave them uninsured, with a two-month-old infant.
Postpartum visits are integral to identifying pregnancy complications early, evaluating them and reducing postpartum complications. The postpartum period is incredibly important for reducing maternal mortality, 45% of total maternal mortality occurs in the first 42 days post birth.15 Medicaid expansion has been correlated with a 17% reduction in hospitalizations during the first 60 days postpartum.16
Through 1115 waivers, states can allow for 12-month continuous eligibility for birthing people. Given the extreme racial disparities in maternal mortality, with Black birthing people three times more likely to die than white birthing people, many leaders believe that extending Medicaid coverage is a step in the right direction towards reducing maternal mortality.17 As of April 2024, 45 States and DC have applied for and gained this extension and several others have taken steps towards adopting the policy.18
Medicaid is more than just a health insurance card, it is a link to vital social services, often the key to improving overall health and well-being, not just health care.
And even if you do not rely on Medicaid for your health care, the Medicaid unwinding can impact you and your family. The COVID-19 pandemic showed us just how interconnected our health is to our neighbors, how important things outside of medicine are to our health and how quickly those of us with stable jobs with health insurance may need Medicaid.
Call to Action: Now more than ever, our health is intertwined with our neighbor’s, we must ensure that everyone continues to have access to medical care and services to ensure a healthy life. This starts with Medicaid. During Medicaid Awareness Month, review and share our resources to support Medicaid and ensure those that need it have the access to the care to which they are entitled.
Have you lost Medicaid coverage recently due to the unwinding? We want to hear from you! Please consider sharing your story to help us fight for better health coverage. You are the voice, the face, and the push behind the policy, your story matters.
Footnotes:
1 https://familiesusa.org/resources/its-time-to-reform-medicaid-eligibility-and-enrollment/
2 https://www.kff.org/policy-watch/what-do-medicaid-unwinding-data-by-race-and-ethnicity-show/
3 https://aspe.hhs.gov/sites/default/files/documents/404a7572048090ec1259d216f3fd617e/aspe-end-mcaid-continuous-coverage_IB.pdf
4 https://www.kff.org/medicaid/issue-brief/implications-of-continuous-eligibility-policies-for-childrens-medicaid-enrollment-churn/
5 https://www.kff.org/medicaid/issue-brief/medicaid-authorities-and-options-to-address-social-determinants-of-health-sdoh/
6 https://www.who.int/health-topics/social-determinants-of-health#tab=tab_1
7 https://www.kff.org/medicaid/issue-brief/medicaid-waiver-tracker-approved-and-pending-section-1115-waivers-by-state/#Table3
8 https://www.commonwealthfund.org/blog/2024/how-medicaid-protects-beneficiaries-financial-stress-and-how-it-could-do-more
9 https://onlinelibrary.wiley.com/doi/full/10.1111/boer.12411
10 https://ideas.repec.org/a/wly/jpamgt/v40y2021i2p348-375.html
11 https://www.healthaffairs.org/doi/10.1377/hlthaff.2019.00931
12 https://www.nejm.org/doi/full/10.1056/nejmsa1212321
13 https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2023.00973
14 https://home.treasury.gov/news/featured-stories/racial-differences-in-economic-security-housing
15 https://www.aafp.org/pubs/afp/issues/2019/1015/p485.html
16 https://www.healthaffairs.org/doi/10.1377/hlthaff.2022.00819
17 https://www.cdc.gov/healthequity/features/maternal-mortality/index.html
18 https://www.kff.org/medicaid/issue-brief/medicaid-postpartum-coverage-extension-tracker/