Medicaid Managed Care: A Multibillion-Dollar Business With Little Oversight
11.08.2023
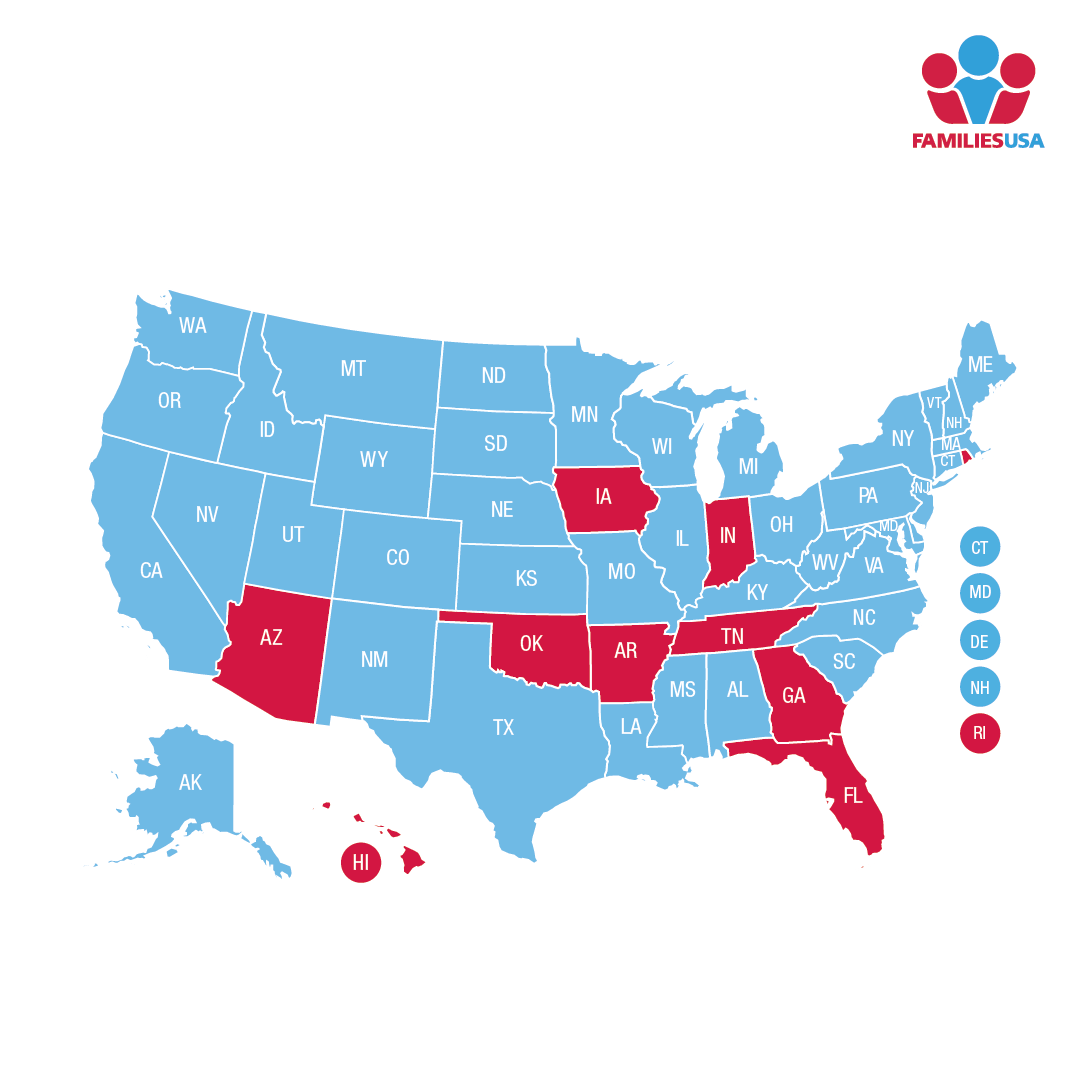
Medicaid managed care organizations (MCOs) are essential to the U.S. health care system and are responsible for delivering health care services through state Medicaid programs to nearly 60 million Americans. As part of their critical role in health care delivery, MCOs are accountable for managing costs, utilization and the quality of care delivered to our nation’s families who rely on Medicaid for health insurance. They contract with state Medicaid agencies and receive capitated payments to maintain provider networks that meet the needs of the patients they serve. Over the last 30 years, the role of Medicaid MCOs in the health care system has expanded significantly, with more than 40 states now relying on MCOs to administer Medicaid benefits. Some states are also leveraging MCOs to coordinate and integrate health care services to improve the health of populations with chronic and complex conditions, and to increase accountability for high-quality care.